Acute care can be challenging and there’s a lot of expectations and things you should know before treating patients.
When I started my first job in acute care, I had little experience and there weren’t a lot of resources to help me feel comfortable and confident.
Today, my hope is that I can help you feel a little more comfortable before getting your feet wet.
Should new grads work in acute care?
Despite what some may say, yes new OTs can start working in acute care. My first job was in acute care, and I had zero experience, but I worked in an acute rehab and felt comfortable evaluating and treating patients.
Acute care is much more fast paced than acute rehab and many of the patients have more critical needs. You’ll have more lines to manage, precautions to consider, and the knowledge doesn’t accumulate overnight.
It’s best to have a mentor to guide you for your first week, and when you start working in the ICU, make it gradual. The ICU can be the most intense place for a new grad and much of it can go right over your head. I recommend spending a significant amount of time co-treating with another PT or OT until you feel more comfortable.
Benefits of working in acute care
Here are a few reasons to work in acute care.
- Patients are not typically scheduled
- More flexible schedule for therapists
- Better benefits working in a hospital
- Opportunities for growth
- Easier treatment times with patients
- Less pressure to see patients who aren’t appropriate for therapy
How much experience do you need?
If you’ve never worked in acute care, I would recommend at least some kind of experience in acute rehab or a skilled nursing facility, or just take some courses here.

You need to know how to evaluate and treat a patient, when it’s safe to see a patient, and when it’s not safe to see a patient.
Some acute care facilities will have guidelines or protocols specific to a diagnosis. Other locations may expect you to be comfortable and confident without any assistance.
Always make sure there’s someone that can help if you have questions or concerns about seeing a patient.
What precautions should I take?
Before you see any of your patients you should review the medical chart, doctor’s orders, imaging, labs, operative report, pertinent medications, and respiratory status.
Here’s a list of all the things you might review in the patient’s chart before seeing them for therapy.
- Activity orders to see if the patient is safe to be out of bed
- Orders for splint or brace
- Orders for ROM or exercises
- Weight bearing status
- Recent Surgeries
- Critical lab values
- Imaging
- Medications
- Vitals
The medical chart is helpful, but it doesn’t tell the entire story. Check with the nurse and ask if the patient is appropriate for therapy.
See if the nurse is okay if you assist the patient out of bed or up in a chair. Ask if the patient has an IV that can be disconnected.
When seeing the patient, ask how the patient is feeling and if they’re willing to participate with therapy. Check vitals and notice how the patient is breathing.
Functional Mobility
Always check that the doctor’s orders allow you to get the patient out of bed. If you’re seeing an orthopedic patient, see if there are any specific orders regarding weight bearing or precautions related to ROM or bracing.
UCLA has a great article on assessing bed mobility by using the BMAT tool. It’s a quick way to assess if the patient is ready for next step in functional mobility.
When assessing bed mobility, use the bed to your advantage. I always bring the bed level to my height, so I’m not bending when I assist the patient from supine to sit.
If the patient is unable to get out of bed without Max or Total Assist, most beds have a chair mode function. You might also use a lift.
At the bottom of this article, there’s a list of precautions to consider before working with a patient in acute care.
How to do an acute care evaluation?
Start by gathering information related to the patient’s recent functional abilities and move on to assess ROM, strength, functional mobility, and ADLs. For more complex patients, you may need to assess cognition, vision, and neurological findings.
Occupational Profile/History
In acute care, we don’t always have time to gather a complete occupational profile. Here’s a list of questions you will need to ask your patient.
- Who do you live with?
- Are they able to care for you?
- Do you have stairs
- What type of dwelling?
- Level of assist needed to perform ADL prior to admission
- Do you have a walk in shower or tub shower
- Do you have a shower chair and grab bars
- Any other DME (Walker, BSC, cane, etc)
- Level of assist needed to perform IADL
- Working?
- Driving?
- Can you meal prep?
- How do you do your grocery shopping?
Here are some components you may want to include in your evaluation.
- Vitals (Orthostatic BP, O2, HR, temperature)
- ROM and MMT (Manual muscle testing)
- Functional mobility assessment
- Ability to perform ADL (feeding, oral hygiene, dressing, toileting, etc)
- Cognition screening (Modified MOCA or clock test)
- Visual assessment (Neglect, visual field cut, tracking, etc)
- Neuro assessment (proprioception, fine motor, gross motor, tone, etc)
Depending on your diagnosis, your evaluation may differ. You likely won’t evaluate your orthopedic patients the same as your neurological patients.
Acute care treatment
A typical treatment session in acute care is typically 45 minutes. Sometimes more or less, depending on what the patient can tolerate.
For treatment, you should be working on the goals in your plan of care. This usually includes ADLs but you might also perform activities to address
- Cognition
- Strength and ROM
- Fine and gross motor coordination
- Neuromuscular reeducation
- Vision
You might also add additional assessments as part of your treatment to screen cognition, vision, neurological deficits, etc.
Your number one goal is to help the patient work on activities to help them return to functional independence. If the patient is not progressing or meeting goals, you may need to discharge the patient from OT services. You should also educate family members and caregivers on activities for long term care such as ROM, repositioning, transfers, and ADLs.
How to do an SOAP note in acute care
Acute care documentation is a little different than acute rehab and skilled nursing. The most important information for the doctor, nurse, and case manager is your discharge recommendations.
Your assessment should convey why the patient is appropriate for your discharge setting. To learn how to write an acute care SOAP note with examples, read my other post here.
The difference between working in acute care and acute rehab
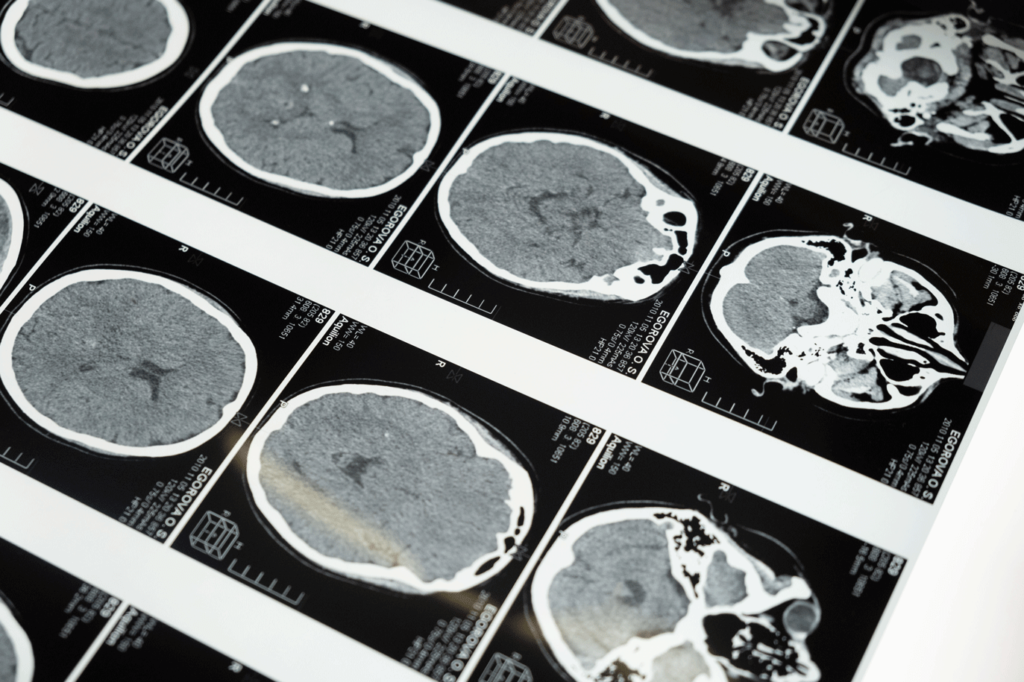
Precautions
Acute care tends to have more precautions than acute rehab, because the patient’s are less stable and have more acute injuries. You may still need to be looking for these precautions in acute rehab, but you don’t have to worry as much when seeing your patient for therapy.
The most important precautions in acute care are if the patient is stable enough to be seen by therapy. Here are some reasons why you should not see a patient in acute care.
- Low hemoglobin
- Brain imaging with active bleed or mass effect
- Low oxygen without mobility
- Increased agitation or combative
- Critical labs (INR, sodium, hgb, troponens)
- Troponin levels are trending up
- Femoral Artery line
- DVT without blood thinners
- Vomiting/diarrhea
- Unstable spinal cord injury
- Recent lumbar puncture
- Recent sheath removal
- Pulmonary Embolism (untreated)
- New onset of Chest pain
- Labored breathing
- Heart rate greater than 130
I can’t name all the reasons why you shouldn’t see a patient, and this is why you should always check with the doctor or nurse before seeing a patient.
If you’re ever concerned about seeing a patient, always check with the doctor. The nurse can be helpful, but if something goes wrong and you didn’t consult the doctor, you may be liable for malpractice.
Work Pace
If you’ve worked in acute rehab, you notice the pace is much slower. You may spend 60-90 minutes with a patient in acute rehab and spend only 30-45 minutes with a patient in acute care.
It can be challenging to spend 90 minutes with a patient who doesn’t want to do therapy. Everyone is different, but that’s why I prefer to do acute care.
Conclusion
Acute care can be challenging, but I can’t think of a more rewarding place to start a career in OT. The learning opportunities in acute care are unlimited, and it really doesn’t take long to feel comfortable and confident.
If you want to improve your skills in acute care or other OT settings, take a course from Medbridge and apply my promo code OTFOCUS to get $175 off.
They have a ton of courses related to acute care and they’re unique because they have resources for patients.

I hope you found this article to be helpful. Subscribe below to learn more OT tips and tricks.

David is the lead editor of OT Focus. He has been practicing as an Occupational Therapist since 2013. He specializes in acute care, hand therapy, and ergonomics.




